Mapping Vaccine Hesitancy: Country-Specific Characteristics of a Global Phenomenon
Institut national de santé publique du Québec - INSPQ (Dubé, Gagnon); Centre de recherche du CHU de Québec (Dubé); Université Laval, Québec (Dubé); World Health Organization - WHO (Nickels, Jeram, Schuster)
"Vaccine hesitancy is an individual behaviour, but is also the result of broader societal influences and should always be looked at in the historical, political and socio-cultural context in which vaccination takes place."
At the request of the WHO Strategic Advisory Group of Experts (SAGE) on Immunization (see Related Summaries, below), researchers carried out an interview study with immunisation managers (IMs) to better understand the range of vaccine hesitancy determinants that are encountered in different settings. In order to map the influential contributing factors, the SAGE Working Group developed a matrix of determinants of vaccine hesitancy based on a systematic literature review. It differentiates between contextual, individual, group, and vaccine- or vaccination-specific factors that influence the acceptability for vaccination.
Using a guide developed by SAGE, between September and December 2013, the researchers conducted telephone-based interviews with IMs in 13 selected countries from the 6 WHO regions were conducted; most represented low- and middle-income countries (n = 11). Vaccine hesitancy was not defined consistently by the IMs, and most interpreted the term as meaning vaccine refusal. (See Table 1 for a summary of IMs' opinions on vaccine hesitancy.) Even if there had been reports of vaccine hesitancy in their country, 11 of the 13 IMs considered that vaccine hesitancy was not common and that it did not have a significant impact on vaccine uptake in routine immunisation (RI) programmes. IMs from two countries indicated that mass immunisation campaigns, rather than RI programmes, were affected by vaccine hesitancy. Factors concerning convenience and ease of access were perceived to be important by 9 of the IMs (see Table 2). Convenience was a factor for sub-populations which did not use the health services provided and for hard-to-reach populations. For instance, in one country, more than 25% of the population had no access to health services, and access was difficult for immigrants, refugees, nomad populations, those living in remote areas, and for women (mainly because of the socio-norms that require them be accompanied for travel to obtain health care).
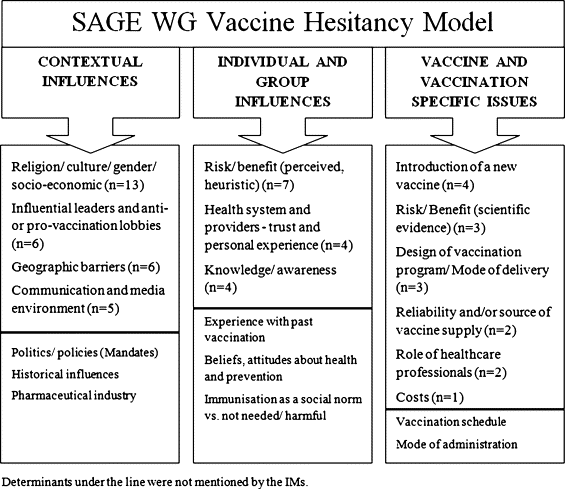
Figure 1 summarises the opinions of IMs regarding the main determinants of vaccine hesitancy in the Working Group matrix.
- In terms of contextual influences, religious beliefs were often a causal factor in vaccine hesitancy (cited by 9 IMs). Several IMs were able to specifically identify religious groups in their country that were known to be opposed to all vaccines, while others discussed "religious reasons" without specifying a religion or a group. Causes of vaccine hesitancy linked to the "communication and media environment" were identified by 5 IMs. Two IMs spoke broadly about "rumours and misconceptions" regarding vaccination circulating in their country, and 3 directly identified negative information conveyed in the mass media (television and internet) as causes of vaccine hesitancy. Geographic barriers and hesitancey seen among those without an official status were also mentioned.
- In terms of individual and group influences, risk perceptions were identified by 7 IMs as causal factors. This included concerns regarding vaccine safety, lack of perceived benefits of vaccination, and lack of understanding of the burden of vaccine-preventable disease. People's level of trust in the health system and health-care providers was identified by 4 IMs as a causal factor. Lack of knowledge (or misinformation) in the population regarding vaccination was identified by four IMs as a contributing factor in vaccine hesitancy.
- In terms of vaccine- and vaccination-specific factors, risk of adverse events following vaccination was identified by 3 IMs as contributing to vaccine hesitancy. Lack of knowledge about vaccination among health professionals was specified by 2 IMs.
Overall, the researchers found that causes of vaccine hesitancy varied in the different countries and were context-specific, indicating a need to strengthen the capacity of national programmes to identify the locally relevant causal factors and to develop adapted strategies to address them. They note that "IMs may need not only to carry out a country assessment of hesitancy, but also a subnational and even a district level assessment, to fully understand the extent of the phenomenon within a country. This will be particularly important when planning for supplementary immunization activities, surveys, or specific campaigns to catch up the non-vaccinated or under-vaccinated, for which vaccine-hesitant persons could be selected as a specific target group." They stress that this research has highlighted the need to ensure that health professionals and those involved in immunisation programmes are well informed about vaccine hesitancy and are able to identify and address its determinants.
The results of this study will be used by the SAGE Working Group on vaccine hesitancy in preparing its recommendations to the SAGE, which will then consider potential global health policy implications.
Vaccine, Volume 32, Issue 49, 20 November 2014, Pages 6649-6654
- Log in to post comments












































