Exploring Factors Improving Support for Vaccinations among Polish Primary Care Physicians
National Institute of Public Health-National Institute of Hygiene (Stefanoff, Augustynowicz); Norwegian Institute of Public Health (Stefanoff); University of Warsaw (Sobierajski); Warsaw University of Technology (Bulinska-Stangrecka)
"Future research is necessary to understand the determinants of low confidence in both vaccinating physicians and all HCWs [health care workers]."
A large-scale European Union (EU) investigation of vaccine confidence highlighted that between 2015 and 2018, Poland noted the largest decrease in public confidence in the importance, effectiveness, and safety of vaccines. Previous research revealed that Polish residents have a positive overall perception of vaccinations but poor knowledge of vaccines and vaccine-preventable diseases (VPDs), as well as concerns about vaccine safety. These studies also highlighted the role of primary care physicians (PCPs) as the most used and the most trusted source of information on vaccination for parents. In this context, the present study explored factors influencing support for vaccinations among physicians employed in the national childhood immunisation programme in order to inform education of healthcare workers and programme organisation.
In June-July 2017, the researchers carried out a national cross-sectional survey of physicians working in randomly selected primary healthcare practices, interviewing 500 of them by telephone using structured, anonymous computer-assisted telephone interviews (CATI). Key findings:
- The most commonly used sources of information on vaccinations were scientific literature and manuals (72%), scientific training courses (53%), internet resources (websites and social media, 23%) and official documents from public health institutions (13%).
- 461 (92.2%) physicians followed recommendations of the childhood immunisation programme by offering recommended vaccinations and informing parents about possible adverse events following immunisation (AEFIs).
- The average self-assessed knowledge (range 0-5) was 4.31 (SD 0.61). The score based on addressing anti-vaccination myths (range 0-3) was 2.34 (SD 0.82). There was no correlation between the self-assessed knowledge and addressing anti-vaccination myths.
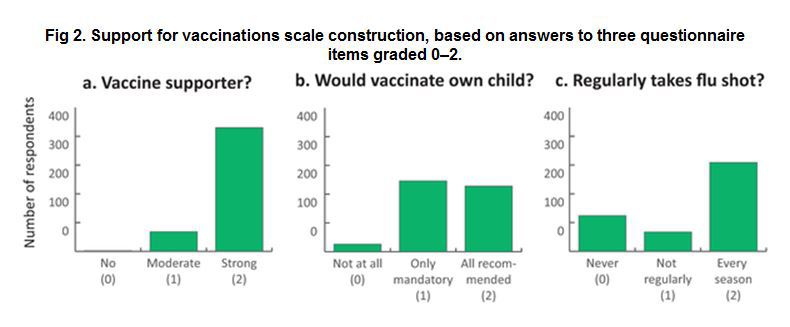
- The median vaccination support score (0-6) was 5 (interquartile range (IQR) 2). 86% of respondents described themselves as strong supporters of immunisations; 46% declared that if confronted with the decision to vaccinate of their own children, they would decide to give them all mandatory (reimbursed by the state) and recommended (paid) vaccinations. Each year, 62% took the recommended vaccine against seasonal influenza.
- After adjusting for other variables, there were no significant effects on vaccination support score on the following: sex, medical specialty, adherence to recommendations, attendance of a conference in the previous year, use of non-scientific sources of information, or self-assessed knowledge.
- Age over 60 years, correct addressing of vaccination myths, and use of one or more than one scientific sources of knowledge significantly improved support for vaccinations.
- A near 10% subgroup of vaccinating physicians seemed to have doubts about the safety of vaccines. Comparing the 42 physicians whose support for vaccination was lowest (score of 2 or below) with remaining respondents, the least supportive PCPs agreed more frequently that the barrier for informing parents about vaccinations was lack of arguments to address parents' concerns (19% vs. 12%, p = 0.172) and identified less frequently as a barrier their own communication skills (2% vs. 9%, p = 0.125). None of the differences in the barriers for informing parents about vaccinations were statistically significant. Compared with remaining respondents, the least supportive PCPs more frequently agreed with vaccination myths, especially those related with vaccine safety.
In reflecting on the findings, the researchers note that "Exclusive use of scientific sources of information and addressing vaccination myths were most strongly associated with vaccination support. These associations could result both from the positive role of knowledge of vaccines and immunisation, and from the possible ambiguous influence of non-scientific sources of information, like opinions of colleagues, opinions of patients, websites and/or social media. The association between knowledge and vaccine confidence among healthcare workers (HCWs) has been documented previously...Future research in Poland should therefore address improved accessibility of evidence-based information on vaccines and vaccine-preventable diseases, including both the appropriateness of contents and of communication channels for different healthcare groups."
In conclusion, the researchers recommend increasing the amount, quality, and accessibility of evidence-based educational materials for PCPs working with childhood immunisations. As a long-term measure, they advise the revision of graduate and post-graduate curricula of healthcare workers training to include more vaccinology content.
PLoS ONE 15(5):e0232722. https://doi.org/10.1371/journal.pone.0232722
- Log in to post comments












































