Vaccine Confidence and Hesitancy in Brazil
Faculdade São Leopoldo Mandic (Brown, Sperandio, Turssi, Leite, Berton, Succi, Napimoga); London School of Hygiene and Tropical Medicine (Larson)
The aim of this study was to assess vaccine confidence and hesitancy in Brazil, where measles-mumps-rubella (MMR) vaccine coverage has been dropping steadily since 2013, causing concerns that pockets of unimmunised people may be growing nationwide. One persisting driver of vaccine reluctance is the issue of mistrust, as was seen, for example, in the Northern Nigerian boycott of the polio vaccine in 2003-2004. The consequence of that distrust - not accepting vaccination - had negative public health impacts and significant costs to the Global Polio Eradication Initiative (GPEI). The state of vaccine confidence, as investigated via the Vaccine Confidence Index (VCI) questionnaire, developed by the Vaccine Confidence Project (VCP), had not been formally assessed in Brazil. The intention of the VCP's global mapping effort is to detect signals and identify trends and changes across countries, like Brazil, so they can be investigated and understood, and so strategies can be developed to address them at an early stage.
Data collection consisted of both online and face-to-face interviews with 952respondents in Brazil carried out between February and July 2016. The study population was a convenience sample, defined as non-probabilistic and therefore not necessarily representative of a certain area or region. The interviews were guided by a general questionnaire regarding perceptions on vaccines and vaccination; further exploratory questions were used with the subset of respondents (352) who were parents of children aged under 5. Such questions extracted information regarding vaccination behaviour, opinions on vaccination and government health services, and vaccine hesitancy.
The overall hesitancy rate was 16.5% (n=157), and the refusal rate was 4.5% (n=43). Eighty-one (23%) of the 352 parents with children under 5 were hesitant regarding vaccinating their children and 6 were outright refusers (7.4% of the hesitant people). Overall, confidence in immunisation was higher than confidence in family planning services, community health workers, and Brazilian Unified National Health System (SUS) emergency services. Although 153 (43.6%) parents with children aged under 5 years indicated high confidence in immunisation, among the 75 (21.3%) who were hesitant, 26 (7.4%) still had high confidence in immunisation. The highest percentage of reasons for hesitancy was attributed to confidence issues: 41.4% and 25.5% did not believe the vaccines were safe or effective, respectively. Hesitancy due to concerns about adverse events - a more concrete way of framing "safety" - accounted for 23.6%.
The sociodemographic analysis revealed that both ends of the socioeconomic spectrum are somewhat hesitant towards vaccines, but possibly for different reasons. Overall, respondents were less likely to be hesitant or refuse vaccination if they were older than 45 years, not single, earning more than one minimum wage per month, and more educated. The researchers suggest that factors other than education and wealth may influence people at this end of the socioeconomic spectrum, e.g., religious beliefs, preference for naturopathy/homeopathy, and easy access to online discussion forums promoting anti-vaccination views.
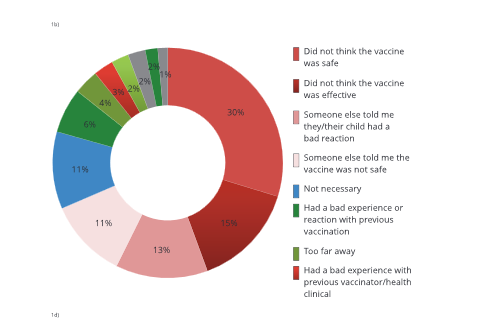
When comparing the reasons for hesitancy between people who did go on to get the vaccine and people who ultimately refused it, with those who did vaccinate, the top 5 reasons for hesitancy were: (1) did not think the vaccine was safe; (2) did not think the vaccine was effective; (3) had a bad experience or reaction with previous vaccination; (4) someone else told me they/their child had a bad reaction; and (5) someone else told me that the vaccine was not safe. For those who did not vaccinate, the top 5 reasons for hesitancy were: (1) did not think the vaccine was safe; (2) did not think the vaccine was effective; (3) not necessary; (4) someone else told me they/their child had a bad reaction; and (5) other beliefs/traditional medicine.
Overall, vaccine confidence using the VCI in this sample of the Brazilian population was similar to that reported previously, which shows high confidence levels, though a clear trend toward lower levels of confidence was associated with higher levels of hesitancy. Amongst the reasons for vaccine hesitancy, the answer "not necessary" was given by 10 of the 122 hesitant respondents, which suggests a degree of complacency mixed in with possible confidence issues. This finding differs from previous reports for countries such as the United Kingdom, India, Pakistan, and Georgia.
The researchers conclude that, despite overall vaccine confidence being high, a clear trend toward lower levels of confidence was associated with higher levels of hesitancy, which warrants ongoing monitoring, due to the dynamic and changing nature of vaccine hesitancy. The researchers indicate that tailored and specific strategies should be developed to engage hesitant publics, health providers, and policymakers in Brazil.
Cadernos de Saúde Pública 2018; 34(9):e00011618. doi: 10.1590/0102-311X00011618
- Log in to post comments












































